The fibrous dysplasia (Jaffé-Lichtenstein disease) is a malformation of the bones. It mainly occurs in children and adolescents. Instead of growing properly and developing a firm, mineral structure, individual bones form fibrous tumors. Therefore, fibrous dysplasia is sometimes referred to as a “tumor-like bone lesion”. Here you will learn everything important about this disease.
Fibrous dysplasia: description
Fibrous dysplasia is a congenital disorder in which one or more bones do not develop in their normal cell structure; instead, tumors of fibrous connective tissue arise. Most commonly, this happens on a femur, but shin, rib, skull and jaw bones are also relatively often affected.
The fibrous dysplasia is based on a genetic defect, but is not hereditary. Male and female sufferers are more or less in balance, with multiple affected bones (polystotic fibrous dysplasia) appearing more often in girls. Children and adolescents between the ages of 5 and 15, and less often adults, are the most affected.
Although it is one of the most common bone diseases, fibrous dysplasia is a rare disease overall. Exact numbers are not known, however, as the fibrous dysplasia in many cases runs without noticeable symptoms; Physicians therefore assume that they are often not diagnosed.
Fibrous dysplasia: different manifestations
Doctors distinguish different forms of the disease:
- monostotic fibrous dysplasia (70%): only one bone is affected
- polystotic fibrous dysplasia (25%): multiple bones are affected
- McCune-Albright syndrome (very rare): fibrous dysplasia with café au lait spots and premature sexual maturity
The McCune-Albright syndrome is often listed as a separate disorder but is based on the same genetic basis as the fibrous dysplasia remains without any conspicuous symptoms.
Fibrous dysplasia: symptoms
The fibrous dysplasia can be very different; Therefore, the symptoms also differ depending on the severity and on which bones are affected. While some sufferers are completely symptom-free, others have different symptoms:
- easy pulling bone pain
- Stress pain (for example, in affected thigh bone)
- Difficulty walking, so that some sufferers even limp
- frequent spontaneous fractures in actually light load (fatigue fractures)
- externally visible “bumps”, bends and other changes in the bones (e.g., a visibly deformed facial skull)
- rapid physical development in affected children and adolescents (rapid growth and early puberty)
- Pigment disorders, so-called café au lait stains
The last two symptoms belong to the so-called McCune-Albright syndrome; very few people with fibrous dysplasia are affected. Café au lait stains are uniformly light brown, sharply defined spots, which also occur, for example, in the hereditary disease neurofibromatosis type 1 (Recklinghausen disease). In McCune-Albright syndrome, they often focus on one half of the body – as does fibrous dysplasia or its affected areas (“foci”). Premature puberty is due to a change in hormone balance. Sometimes, fibrous dysplasia also occurs in association with other hormonal diseases such as diabetes, Cushing’s disease or hyperthyroidism.
Fibrous dysplasia: causes and risk factors
The fibrous dysplasia is due to a change in the genome: the so-called GNAS gene of the 20th chromosome is changed (mutated). As a result, the enzyme adenylate cyclase produces too much cAMP (cyclic adenosine monophosphate), a specific substance that plays an important role in signaling in the cell. Ultimately, the mutation causes the spongy inner layer of the bone – the so-called spongiosa – is not properly formed. In its place is a soft, non-mineralized, connective tissue-like bone substance (osteoid). The cells divide before they are properly differentiated, causing the bone to be literally distended.
The genetic defect affects only body cells and not the germ cells – one speaks of a somatic mutation. Presumably, the gene mutates during embryonic development or early childhood, so the mutation is not in the genetic material from the beginning. This means that the GNAS gene defect is not hereditary.
Fibrous dysplasia: examinations and diagnosis
To diagnose fibrous dysplasia, the doctor first inquires about the symptoms and the symptoms medical history (Anamnese). For example, he asks about possible pain, in which situations these occur and whether one or more places are affected. In a physical exam, he looks at the conspicuous places and scans them to check for changes. Maybe the doctor will take blood from the victim. In the case of fibrous dysplasia, a normal level of calcium and phosphate is found in the blood serum; for this the enzyme alkaline phosphatase can be increased. This blood count is one of a group of enzymes that can, among other things, indicate changes in bone metabolism.
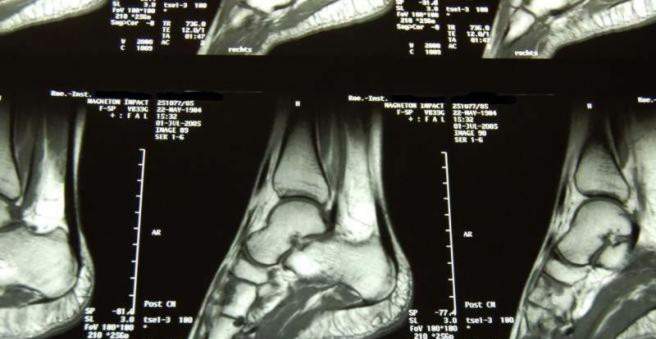
The most important method to diagnose fibrous dysplasia is the X-ray, It is not uncommon for an X-ray to guide the suspicion of the rare disease, for example after a bone fracture. The doctor sees a frequently spindle-shaped, milky glass clouded, thickened spot in the affected bone, where the bone structure is replaced by connective tissue. Partly the changes look like bone cysts. The outer bone layer (cortical bone) is also usually thinner than in a healthy bone. A Computed tomography (CT) helps the doctor to take a closer look at the changes. The examinee lies in a special device, which produces layer by layer very precise X-ray images of the body in the form of sectional images. Another imaging technique is the bone scan, With this nuclear medicine examination, changes in the bone metabolism can be. If there is a suspicion of polystotic fibrous dysplasia, skeletal scintigraphy will help track down any affected bones (foci).
Even if only a single bone is altered (monostotic fibrous dysplasia), the correct diagnosis by the imaging techniques can sometimes be difficult, as some other diseases are similar (e.g., bone cyst, benign fibrous histiocytoma, hemangioma, chondrosarcoma). In that case, the doctor takes one tissue sample from the altered site (biopsy), which is subsequently examined under the microscope. In fibrous dysplasia, a typical structure is composed of dense, collagenous connective tissue traversed by small trabeculae of bone tissue (bone trabeculae). On its surface are found only a few “original bone cells” (osteoblasts), but radially arranged collagen fibers.
Fibrous dysplasia: treatment
A causal treatment is not possible with fibrous dysplasia. If the femur or tibia is affected, it may be useful to relieve the bone with a splint, for example. So you can prevent possible bone fractures at the unstable places. However, this should be discussed with an experienced orthopedist, as it sometimes comes in the growth of further bone deformities. Therefore, it may be better to strengthen the surrounding bones and muscles as part of a physiotherapy with strength exercises.
If the fibrous dysplasia causes severe pain, it can be contained with painkillers (analgesics). A relatively new therapeutic approach is so-called bisphosphonates – drugs that are also used to treat osteoporosis and other bone diseases. They appear to have a positive effect on the bone pain and fracture tendency accompanying fibrous dysplasia.
In rare cases, the fibrous dysplasia is so pronounced that, for example, bones in the face are severely deformed; then surgery can make sense for aesthetic reasons.
Fibrous dysplasia: disease course and prognosis
The fibrous dysplasia has a total of one good prognosis, The course can be slightly different. In some patients, the herd increase in the course of puberty in batches, so that the affected bones are further distended; however, usually no new flocks are created. At the latest in adulthood, however, the fibrous dysplasia usually comes to a standstill and the bone is not rebuilt.
That fibrous dysplasia develops into a malignant bone tumor (osteosarcoma) is very rare and occurs in less than one percent of cases. Likewise rare are heavy courses, if about the fibrous dysplasia the skull bones are affected and they are deformed so that they limit the function of the brain.