A varicocele (varicocele testis) is a varicose vein on the scrotum. The venous plexus at this point is touch or visibly expanded. Pain and heaviness on the affected side of the testicles may or may not occur. The varicocele can usually be treated by a small procedure. Find out here about causes, symptoms, diagnosis and treatment of varicocele!
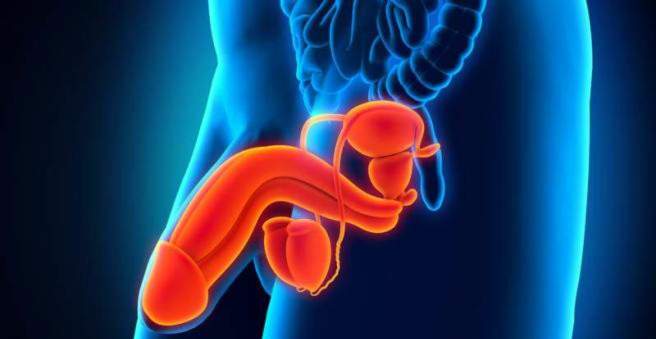
Varicocele: description
The varicocele is a varicose vein extension of the venous plexus (pampiniform plexus) of the testicle. In almost 90 percent of the cases, the extension is on the left side of the testicle. The main causes of a varicose vein break are a weakness of the venous valves, which are intended to prevent blood backflow, or a drainage obstruction. In addition to this so-called primary form of the varicocele, there is also a secondary (or symptomatic) form that expresses another disease, such as a tumor.
The testicular vein (spermatic vein or V. testicularis) carries the blood from the testes into the inferior vena cava with its left and right branches – either directly (right testicular vein) or indirectly via the left renal vein (left testicular vein). If this drain is disturbed at any point, the blood in the testicle builds up. As a result, the vessels expand and a varicose vein develops.
Testicular varicose veins can lead to infertility if left untreated. Thus, one third of all cases of infertility is caused by a varicocele.
Varicocele: frequency
Overall, 30 percent of men have a varicocele. Particularly affected are 14- to 25-year-old men. In childhood, the varicocele is rather rare. In older patients with a varicocele, a precise diagnosis is necessary, as it is usually so-called secondary or symptomatic varicocele. In this case, a tumor as the cause of the varicose vein fracture must be excluded.
Varicocele: symptoms
The varicocele is often symptomless and a chance finding in an investigation.
In some cases, however, the typical symptoms of varicocele also appear: one (felt) heavier, tense and full of scrotum. Particularly intense are the varicocele pain when standing. On the scrotum worm-like swellings are visible, which are visible either with or without increased abdominal pressure during pressing. The testes on the affected side may be smaller, especially in children, by inhibiting growth. This is an indication of a disturbed sperm production. In extreme cases, no sperm are produced (complete infertility).
Varicocele: causes and risk factors
Physicians distinguish a primary and a secondary varicocele.
Primary (idiopathic) varicocele
The primary (idiopathic) varicocele is conditional. It makes up the vast majority of cases of varicose veins and is especially on the left. The reason: The left testicular vein opens at a right angle into the left renal vein (which then leads to the inferior vena cava), which impedes blood flow and promotes backflow. In contrast, the right testicular vein opens at a more acute angle directly into the inferior vena cava (the acute angle is more favorable for the blood flow).
Common cause of the blood backlog is a defect of the venous valves in the testicular vein or a congenital vascular wall weakness. Also, venous drainage due to increased vascular pressure can lead to a primary varicocele. The increase in pressure can be caused by the fact that the left renal vein is trapped between two large arteries (nutcracker phenomenon). The resulting blood backlog can affect the testicular veins.
Secondary (symptomatic) varicocele
The secondary or symptomatic varicocele can be bilateral. It is usually caused by a tumor-related drainage. This is, for example, a tumor of the kidney, the renal pelvis or the ureter. Also, a blood clot (thrombus) or rupture (rupture) in the testicular veins is a possible cause of a secondary varicocele.
infertility
In both the primary and secondary forms there is a decreased blood backflow from the testes. The blood in the testicles flows more and more slowly. This warms the testicles, which affects sperm production and quality. Infertility (infertility) can arise.
In addition, on the one hand, the axis of the testicular-associated hormones (such as FSH – follicle-stimulating hormone) may be disturbed. On the other hand, hormones of the adrenal glands can enter the testicles due to blood backflow or even blood reflux, causing damage there.
Varicocele: examinations and diagnosis
Specialist for diseases of the testicle and thus also for the varicocele is the urologist. In conversation with the patient (anamnesis) he first records the symptoms. Possible questions include:
- Does your testicle feel heavy or swollen?
- Are the symptoms worse when standing?
- Do you have pain?
Physical examination
Then the doctor will first examine the testicle while standing. Due to gravity, the varicocele is usually distinct. If this is not the case, the patient is asked to increase the pressure in the abdomen by pressing or tightening the abdominal muscles. As a result, the swelling of the vessels is often easier to see.
In the next step, the patient lies down. In a primary varicocele, the vascular pattern on the testicle will spontaneously diminish by lying down, meaning that the vessels will empty due to gravity. If this is not the case, it is suspected that it is a secondary varicocele.
Ultrasound
Another important diagnostic step in a varicocele is an ultrasound examination (sonography) of the testicle. The doctor can assess the varicocele more accurately. In addition, the kidneys and the abdomen should be examined ultrasonically – in search of possible explanations for the drainage disorder. To confirm the congestion or even reflux, a test should be performed using Doppler sonography, a special form of ultrasound examination.
Hormone and sperm examinations
If you want to have children or suspected infertility, further investigations should be done. Thus, the determination of hormones and the closer examination of sperm status (spermiogram) in patients with testicular varicose veins is recommended. Testicles play an essential role in fertility.
Vascular radiography (phlebography)
If there is a suspicion of vascular malformation, a so-called phlebography is performed: With the help of X-ray contrast media, an X-ray of the vessels is made in order to examine their course and condition.
Varicocele: severity classification
A varicose vein on the testicles can be divided into three degrees of severity:
- Grade I: palpable enlargement of the venous plexus in the testicle when standing; Vessel size <1 centimeter.
- Grade II: palpable vasodilatation without additional pressure; Vessel size 1 to 2 centimeters.
- Grade III: palpable and visible bundle of vessels; Vessel size> 2 centimeters.
Varicocele: treatment
The treatment of a varicose vein in the testes is important for several reasons. On the one hand, the symptoms can be very unpleasant, on the other hand, there is an increased risk of infertility.
There are no medicines for a varicocele. Therapy of choice is instead a mostly minor surgical procedure. It should be done if:
- it comes repeatedly to pain
- the testicle volume has shrunk
- it is a grade III varicocele
- the varicocele is perceived as a disability
There are a number of different methods to treat the primary varicocele. The therapy of the secondary varicocele is dependent on the underlying disease, for example the tumor.
Varicoceles-sclerotherapy
The dilated vessels in the testes can be sclerosed. This means that you inject a substance into the vessels, which “obliterates” them. The blood can drain well over other blood vessels.
The sclerosing agent can be introduced via a catheter. In the so-called retrograde transcatheter sclerosis Under local anesthesia, a catheter is inserted over a groin vein and renal vein to the venous plexus in the testes. Then the sclerosing agent is injected through the catheter. However, in around 30 percent of cases, this form of varicocele therapy does not lead to success.
You can also make a small incision at the level of the penis root and insert the catheter directly into the venous plexus. Again, a sclerosing agent is injected. This is then called antegrade or anterograde sclerotherapy designated.
Vascular occlusion by embolization
Another treatment for a varicocele is to artificially occlude the affected vessel. For this purpose, you can either introduce a tissue adhesive into the vessel or use a tiny spiral.
Operational procedures
As a last resort, surgical procedures are available for a varicocele. The affected vessel is ligated and severed. This can be done, for example, in the context of a larger, open varicocele op or via buttonhole surgery (laparoscopy): In this only a few small incisions are made, over which one introduces the Op instruments.
Varicocele: disease course and prognosis
An early and therefore timely start of therapy is very important in a varicocele. The prognosis after successful treatment is usually good. Although heightened alertness is required, the danger of infertility is mostly banned.
An untreated varicocele leads to severe damage of sperm formation, a reduced testicular volume and a diminished function of the testicle cells (Leydig cell function). However, symptomless varicoceles that have no effect on sperm quality need not be associated with these complications.
In case of already serious sperm damage (azoospermia, oligo-astheno-teratozoospermia) surgical therapy is not promising. In these cases, alternative fertility techniques should be clarified.
A good therapy of varicocele leads to over 80 percent of patients to freedom from pain and an increase in the testicular volume. It is believed that the sperm quality increases again.
The treatment of a varicose vein in the testicles is significant for a few reasons. From one viewpoint, the side effects can be extremely terrible, then again, there is an expanded danger of barrenness.
There are no drugs for a varicocele. Treatment of decision is rather a for the most part minor surgery. It ought to be done if:
it comes over and again to torment
the gonad volume has contracted
it is a grade III varicocele
the varicocele is seen as an inability
There are various techniques to treat the essential varicocele. The treatment of the auxiliary varicocele is reliant upon the hidden infection, for instance the tumor.
Varicoceles-sclerotherapy
The expanded vessels in the testicles can be sclerosed. This implies that you infuse a substance into the vessels, which “crushes” them. The blood can deplete above and beyond other veins.
The sclerosing specialist can be presented by means of a catheter. In the alleged retrograde transcatheter sclerosis Under neighborhood sedation, a catheter is embedded over a crotch vein and renal vein to the venous plexus in the testicles. Then, at that point the sclerosing specialist is infused through the catheter. Nonetheless, in around 30% of cases, this type of varicocele treatment doesn’t prompt achievement.
You can likewise make a little entry point at the level of the penis root and supplement the catheter straightforwardly into the venous plexus. Once more, a sclerosing specialist is infused. This is then called antegrade or anterograde sclerotherapy assigned.