Pfeiffer’s glandular fever (mononucleosis) is a viral disease that affects almost everyone in the course of life. It is usually transmitted through the saliva and therefore also called kiss disease. Often, however, the disease does not break out or go unnoticed. In adults, the symptoms are often particularly severe and can be seen in sore throats, swollen lymph nodes, fever and dullness. Find out about the most important signs, ways of infection and therapies here.

Pfeiffer’s glandular fever: short overview
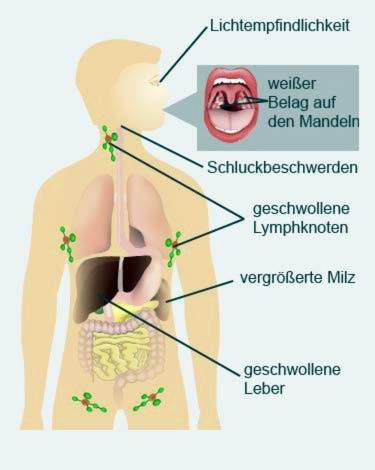
Main symptoms: Sore throat, swollen lymph nodes, fatigue, fever, enlarged spleen
Infection: About the saliva when kissing or about bodily fluids (intercourse, blood)
Diagnosis: Blood test for Epstein-Barr virus (EBV) and EBV antibodies, throat swab, spleen and lymph node scan
Treatment: Symptomatic treatment of pain and fever, severe cortisone
complications: Threatening swollen throat, splenic tear, hepatitis, meningitis, paralysis, rash
Pfeiffer’s glandular fever: symptoms
Pfeiffer’s glandular fever (infectious mononucleosis, mononucleosis infectiosa, monocyte angina) is caused by Epstein-Barr virus (EBV). The disease manifests itself mainly in the form of tonsillitis and pharyngitis with severely swollen lymph nodes, fever and fatigue by Pfeiffer’s glandular fever.
In children, the infection is often symptom poor, since their immune system is not yet strongly responsive to the pathogen. In adults, milder events can be mistaken for a flu infection. But there are also severe courses with complications possible.
Pfeiffer’s glandular fever: main symptoms
Strep throat: Common to Pfeiffer’s glandular fever are severe sore throat with intense reddening of the pharyngeal mucosa and pronounced dysphagia. The tonsils and the lymph nodes swell, some patients get a high fever.
Pronounced languor: Patients feel extremely beaten and powerless in the acute phase of the disease. Most of them recover within a week or two.
In others, however, tiredness, listlessness, and general malaise can persist for a long time-even without the typical symptoms of glandular fever.
In athletes in particular, a sudden weakness is often the first and sometimes the only sign of the disease. In some cases, the pronounced fatigue persists for several months.
Swollen spleen (splenomegaly): The spleen plays an important role in the disease defense and filters dead blood cells from the blood. It is particularly challenged during Epstein-Barr virus infection. In the course of the disease, it can therefore swell and sometimes even rupture.
Pfeiffer’s glandular fever: complications
Mostly, Pfeiffer’s glandular fever is uncomplicated. But it can also cause severe, sometimes life-threatening complications.
Heavily swollen throat: It becomes dangerous when the immune system reacts so strongly to the virus that the pharyngeal mucosa swells up very much. This can make swallowing impossible and even interfere with breathing.
ruptured spleen: A severely swollen spleen may be torn by knocks or drops. Then, the strong internal bleeding creates a life-threatening situation. Patients should therefore strictly avoid the risk of bruising in this condition.
Liver inflammation (hepatitis): The virus can also affect the liver and cause liver inflammation. If this is severe, the skin turns yellow (jaundice) due to impaired liver function in glandular fever.
Skin rash: In about five to ten percent of the patients a spotty, elevated (humped) skin rash forms, the so-called maculopapular exanthem.
Paralysis: If the virus reaches the nervous system, it can trigger inflammation with symptoms of paralysis, which can also threaten respiration.
Inflammations of the brain: The virus can reach the brain. There it can cause a brain or meningitis.
Pfeiffer’s glandular fever: infection and causes
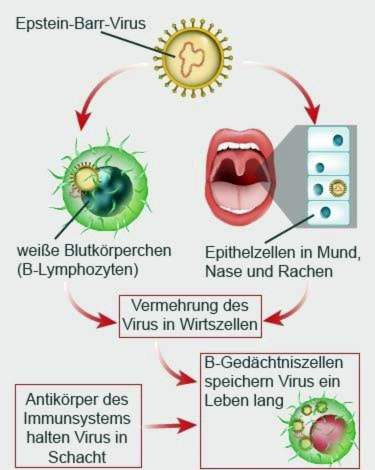
Pfeiffer’s glandular fever is contagious. It is caused by the Epstein-Barr virus (EBV). The pathogen proliferates in the lymphocytes and mucosal cells in the throat. Outside the human body, the virus can not survive long.
routes of infection
EBV is transmitted via body fluids. Since the virus is mainly found in saliva, it is especially easy to get in touch with tight body contact and kisses. In English-speaking countries, therefore, Pfeiffer’s glandular fever is referred to as “Kissing Disease”, also known as “Kiss Disease” in German.
A particularly common way of infection is among infants, such as in kindergarten, where toys often get into the mouth and are interchangeable. Especially “kiss-active” populations such as young adults also become more infected (“student fever”). 95 percent of people over 30 are infected with the glandular fever pathogen.
Other ways of infection, such as sexual intercourse, blood transfusions or organ donation are possible, but much rarer.
Pfeiffer’s glandular fever: incubation period
The incubation period, ie the period between the infection and the onset of the disease, is long in Pfeiffer’s glandular fever. Between infection and outbreak of the disease are usually four to six weeks. In time, however, the infected person can already infect other people, without suspecting that he is ill himself.
How long is Pfeiffer’s glandular fever infectious?
Freshly infected people pass on the virus particularly easily. In this phase, especially many pathogens are excreted in the saliva. This is also the case for a long time after the symptoms have resolved. In order not to infect others, one should therefore be reserved in the first months after the first infection with kissing and avoid unprotected intercourse.
Pfeiffer’s glandular fever-how long is it contagious?
A person who was once infected with the glandular glandular fever remains a life-long carrier of the virus. Although the immune system keeps the pathogen at bay, the disease usually does not break out again.
From time to time, however, the virus is increasingly released into the saliva. Therefore, all virus carriers can infect others for a lifetime even after the symptoms have resolved.
Infection with dysentery glandular fever in pregnancy
There is evidence that primary infection during pregnancy is associated with a higher rate of miscarriages or birth defects. However, most women of child-bearing potential have been infected with Epstein-Barr virus long before pregnancy. Therefore, only a few people get infected during pregnancy for the first time.
If the mother has already undergone an EBV infection, she also transfers her protection against the virus to the newborn. This will last for the first half year of the baby’s life. As a rule, the child can only get infected afterwards.
Pfeiffer’s glandular fever: investigations and diagnosis
The diagnosis of glandular fever is often difficult. Main symptoms such as sore throat, fever and lymph node swelling also occur in simple flu-like infections and colds. In many cases, Pfeiffer’s glandular fever is therefore not recognized at all or only late.
Targeted attention to Pfeiffer’s glandular fever is usually only when the fever does not decrease or the patient complains for weeks of exhaustion or a strong pharyngitis does not subsides.
The main aim of the study is to find out if viruses like the Epstein-Barr virus or bacteria like streptococci cause the symptoms. Antibiotics only help with bacterial infections, but not with viral infections. They would even burden the patient unnecessarily.
Physical examination
Throat Exam: During the physical examination, the doctor will first examine the throat and the tonsils. In glandular fever, they are reddened and often swollen. An indication of the type of infection also provide the coverings: While they look rather stippchenartig in the bacterial streptococcal tonsillitis, they appear white and flat in Pfeiffer’s glandular fever.
Palpation of lymph nodes: By palpation of the neck under the angle of the mandible, the armpits and the inguinal region, the doctor can determine if and which lymph nodes are swollen.
Palpation of the spleen: In glandular fever the spleen swells so much that the doctor can feel it clearly from the outside.
Throat swab: With a throat swab can be determined in the laboratory, whether bacteria are the trigger of the disease. If the smear contains the Epstein-Barr virus, however, it is not enough to diagnose Pfeiffer’s glandular fever. The pathogen can be found not only in an acute infection on the mucosa. It can also be detected if the virus is longer in the body and only reactivated.
Diagnosis by blood test
Antibody: For a reliable diagnosis of Pfeiffer’s glandular fever, specific antibodies against the Epstein-Barr virus in the blood can be detected.
Deformed lymphocytes: A blood test can also be used to determine whether these white blood cells have changed. Since they have to be mass-reformed during the infection, many of them are initially deformed a bit. For this reason they are also called Pfeiffer cells or atypical lymphocytes.
Elevated liver values: If the liver is attacked by the virus, a blood test also shows an increased concentration of liver enzymes (transaminases).
Pfeiffer’s glandular fever: treatment
Pfeiffer’s glandular fever is a viral disease. Antibiotics therefore do not help because they only work against bacterial infections.
Treatment focuses on alleviating ailments such as pain, dysphagia and fever. For this purpose, one uses the common means such as ibuprofen, acetylsalicylic acid or paracetamol.
An important treatment principle in Pfeiffer’s glandular fever is physical rest. This significantly reduces the risk of serious complications. Relief, which includes a strict ban on sport, should be maintained for some time beyond the existence of the acute symptoms of illness.
If complications occur, further treatment may be necessary. If the pharyngeal mucosa swells to a threatening degree, or if symptoms such as fatigue and fever are very pronounced, it is also treated with cortisone or other active ingredients that reduce the activity of the immune system.
A splenic rupture must be operated on immediately, otherwise the patient threatens to bleed to death.
What is still important in the treatment of Pfeiffer’s glandular fever, read in the article Pfeiffer’s glandular fever – treatment.
Pfeiffer’s glandular fever: disease course and prognosis
Pfeiffer’s glandular fever lasts up to three weeks. It usually heals without lasting consequences. However, if there is a suspicion of complications or blood levels deteriorate dramatically, patients are treated for surveillance in the hospital.
In very rare cases the Pfeiffer’s glandular fever becomes chronic. That is, the symptoms persist for months or even years. On the other hand, only very seldom does Pfeiffer’s glandular fever lead to lasting damage due to complications such as liver inflammation and meningitis.
EBV infection is believed to increase the risk of some blood cancers (for example B-cell lymphomas, Burkitt’s lymphoma, M. Hodgkin’s disease).
Pfeiffer’s glandular fever: what you can do yourself
Since the Epstein-Barr virus in the population is very widespread (the “Durchseuchungsrate” is 95 percent), you can hardly protect against it. In the case of a disease, however, you can do a lot to prevent a severe course in glandular fever.
Avoid alcohol
The infection also often burdens the liver considerably. Therefore, you should strictly avoid alcohol in the disease phase in order not to burden the liver additionally. In some cases, the liver values are increased over months, so that regular blood tests are necessary and you should abstain from alcohol even after the symptoms have resolved to avoid permanent liver damage.
Adjust medication
Since many drugs in the liver are broken down, some drugs for the duration of the disease in consultation with the doctor must be replaced by less liver-damaging substances.
Beware of sports!
In the acute phase or in case of severe infections, you should completely abstain from sports, later in consultation with the doctor may be a slight exercise training possible.
If the spleen swells strongly in case of glandular fever, there is the danger that the very blood-rich organ will break when subjected to physical exertion or external violence. The result is severe internal bleeding that can be life threatening. Therefore, contact and martial arts in the acute phase of the disease should be strictly avoided.
Additional information
Book recommendations:
- Underestimated Epstein Barr Virus: What to do in case of chronic EBV infection? (Sigrid Nesterenko, ersa Verlag, 2016)